We recognize that portable power stations can redefine reliability for medical devices by delivering backup, mobile, and resilient energy across care settings. Together, we should map device power needs, interface standards, and lifecycle impacts to minimize downtime and safeguard patient care. As we align safety, compliance, and real-time monitoring with clinical workflows, we’ll uncover practice-ready gaps and opportunities that prompt the next step in our discussion. Let’s explore what matters most here.
Key Takeaways
- Portable power stations ensure continuous operation of life-safety devices and vital monitoring during outages or transport.
- Standardized power interfaces and documented performance enable safe interoperability with diverse medical equipment.
- Lifecycle-aware capacity planning and redundancy support reliable runtimes with predictable margins for clinical workflows.
- Compliance, testing, and auditable records verify safety, isolation, surge protection, and regulatory readiness.
- Real-time power status, maintenance cycles, and escalation workflows integrate with care processes to minimize downtime.
Why Portable Power Matters in Medical Care
Portable power is essential in medical care because reliable energy ensures lifesaving devices function when and where they’re needed most. We approach this topic with precision, outlining how portable power supports continuous monitoring, timely interventions, and patient safety. Our focus is on predictable performance, minimizing downtime, and reducing risk during transport and remote care. Battery longevity emerges as a critical measure: we compare charging cycles, discharge rates, and thermal management to sustain device readiness over shifts and emergencies. Device interoperability then becomes essential: standardized interfaces and compatible power standards enable seamless integration across devices, chargers, and locations. By quantifying endurance, we demonstrate operational resilience and enable informed planning for facility and field use. Together, these factors underpin dependable care delivery, regardless of setting or constraint.
Use Cases Across Care Environments
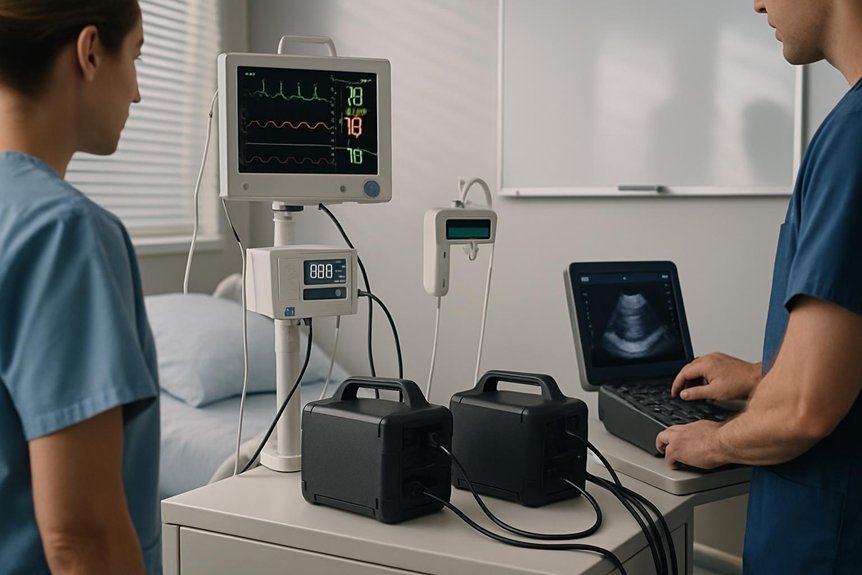
We examine how portable power stations support care across environments, from acute wards to remote clinics, by aligning device power needs with response times and reliability targets. We outline how portable power roles vary—backup, mobile, and resilience—so clinicians can anticipate performance gaps and plan mitigations. This discussion frames concrete use cases that guide implementation and assessment, keeping the focus on safety, uptime, and workflow integration.
Care Environment Scenarios
In diverse care environments, scenarios for portable power stations span clinical facilities, home health, ambulatory services, and emergency response. We analyze how power reliability supports uninterrupted monitoring, life-safety devices, and essential therapeutics. Across settings, we prioritize care ergonomics, ensuring devices are intuitive, accessible, and integrated into workflows without adding strain. We assess standby versus active use, evaluating switchover times, battery capacity, and environmental resilience to temperature, dust, and moisture. Patient interaction remains central: equipment placement, unobtrusive indicators, and clear alarm signaling protect dignity and safety while enabling rapid clinician response. We quantify risk reduction, maintenance cadence, and disaster-readiness through standardized checklists. Ultimately, these scenarios illustrate how portable power stations sustain diagnostic accuracy, treatment continuity, and communication during routine operations and disruptions.
Portable Power Roles
Across care environments, portable power roles translate into explicit use cases that sustain monitoring, support life-safety devices, and enable timely therapeutics. We map each scenario to device compatibility, ensuring that portable power selections align with patient needs and institutional standards. In monitoring zones, portable power maintains continuous telemetry, alarms, and data integrity during outages or transport. For life-safety devices, redundancy and rapid replacement minimize risk to airway, ventilation, and monitoring circuits. Therapeutic workflows benefit from on-site charging and surge protection that preserve medication infusion timing and image-guided interventions. We assess battery chemistry, capacity, and cycle life to forecast maintenance load and downtimes. Our framework emphasizes interoperability, documented performance, and clear escalation paths, guiding procurement, testing, and staff training for reliable device compatibility and uninterrupted care delivery.
Essential Electrical Specs for Medical Devices

Essential electrical specs define the safety and reliability of medical devices powered by portable stations. We outline critical parameters that ensure patient protection and uninterrupted function, focusing on tolerance, stability, and compliance. Our approach ties device performance to portable power characteristics, minimizing risk during outages or mobility. We assess these elements through a disciplined framework: input tolerance, output regulation, and protection mechanisms. Key considerations include preventing overvoltage, managing ripple, and sustaining accurate power delivery under varying loads. We also monitor essential electricals and respond to medical device alerts with rapid verification steps.
- Stable voltage and current within defined ranges
- Robust protection against short-circuits and thermal stress
- Clear labeling, fault indicators, and documented charge cycles
Choose the Right Power Station: Capacity, Ports, Recharge
We’ll start by evaluating Capacity Considerations, ensuring the power station can sustain the device’s critical load without frequent recharges. We’ll compare Port Availability to match the device’s input options and any auxiliary equipment we rely on. Finally, we’ll assess Recharge Versatility to support standby use, rapid recharging, and different energy sources.
Capacity Considerations
How should you choose a portable power station for capacity, ports, and recharge options? We approach capacity by balancing expected device runtime with margin for surge and uncertainty. We emphasize capacity planning to prevent outages and unnecessary swaps, while recognizing battery lifecycle implications: higher-capacity cells offer longer runtimes but add weight and wear patterns. We analyze runtime estimates, efficiency losses, and derating under load, then translate results into actionable thresholds for clinical use.
- Clear runtime targets aligned to patient needs
- Conservative margins to absorb surges and temperature effects
- Lifecycle-aware choices that match device duty cycles
This structured view keeps decision-making precise: quantify use, anticipate degradation, and select a unit that sustains critical functions without overcommitting resources.
Port Availability
Choosing the right portable power station means balancing not just capacity but the mix of ports and recharge options that your clinical setup requires. We assess port availability to support essential devices while avoiding bottlenecks that threaten uptime. We prioritize diverse outputs (AC, USB-C, USB-A, DC) to enable seamless device handoffs and avoid daisy-chaining adapters. We also factor recharging paths that align with patient care cycles, maintaining power redundancy so a single failure doesn’t compromise treatment. Our approach is to map required devices to port types and verify that critical lines have direct, redundant feeds. Below, a concise reference helps compare options at a glance.
| Port Types | Redundancy Scenarios | Observed Fit |
|---|---|---|
| AC / USB-C / DC | N+1 resilience for key devices | High adequacy |
Recharge Versatility
Recharge versatility hinges on aligning capacity with recharge options and port availability to sustain patient care cycles. We evaluate how quickly a unit can restore power after use and how its recharge pathways fit hospital rhythms, from rapid recharges between rounds to banked energy for off-site care. Our approach emphasizes portable adaptability: selecting stations that mirror device energy profiles and procedural tempo, ensuring continuous operation without depleting critical reserves.
- Capacity vs. recharge rate alignment for uninterrupted cycles
- Port mix and accessibility to support multiple devices simultaneously
- Recharge scheduling that fits clinical workflows and transport constraints
This framework guides decisions toward balanced, data-driven choices, prioritizing reliability and flexibility. By focusing on recharge versatility and portable adaptability, we optimize care continuity and staff efficiency across settings.
Safety and Compliance in Medical Power
Safety and compliance in medical power is nonnegotiable: we must verify that portable power stations meet applicable medical device standards, regulatory requirements, and performance specifications before deployment. Our evaluation focuses on Safety compliance, risk mitigation, and traceability, ensuring devices remain within labeled limits during use. We assess electrical safety, isolation, leakage, and arc-fault protection, alongside compatibility with monitored patient environments. We analyze battery lifecycle to anticipate degradation risks, maintain performance, and support device reliability over time. Documentation, testing protocols, and supplier qualifications underpin our governance, reducing supply chain uncertainty. We require clear maintenance plans, timely recalls, and auditable records for accountability. By aligning with standards and validating performance, we protect patients, clinicians, and operations while sustaining uninterrupted medical power.
Incorporating Portable Power Into Care Workflows
- Real-time power status prompts aligned with clinical cues
- Lightweight, patient-centric accessories that minimize disruption
- Redundant pathways for essential devices during transitions
Maintenance and Reliability: Real-World Questions
How reliable are portable power stations in real clinical settings, and what maintenance practices best prevent downtime? We address this with a structured approach, focusing on maintenance reliability and how it translates to clinical uptime. We evaluate failure modes—battery degradation, inverter faults, and connection wear—and quantify their impact on device performance. Preventive protocols include regular cycle testing, firmware checks, voltage and temperature monitoring, and documentation of usage history to identify trends. Real world questions center on environmental exposure, charging discipline, and reporting latency when alarms trigger. We recommend standardized checklists, rapid root-cause analysis, and supplier SLAs that cover diagnostics and replacement parts. Ultimately, reliability hinges on proactive maintenance, disciplined data capture, and timely responses to evolving field conditions.
Budgeting TCO for Healthcare Power
What is the true total cost of ownership (TCO) for healthcare power solutions, and how do we quantify it across clinical, operational, and decommissioning phases? We, as a team, map budgeting tco to observable cost drivers, separating upfront capital from ongoing expenses and end-of-life costs. This framework clarifies tradeoffs between reliability, maintenance intervals, battery lifecycle, and downtime risk. We identify concrete cost drivers in each phase, enabling disciplined budgeting and scenario testing.
- Procurement and capital outlay, including unit cost and financing
- Operational expenses, service, replacements, and energy efficiency
- Decommissioning, disposal, and regulatory compliance costs
Frequently Asked Questions
How Do Portable Power Stations Handle Hospital-Grade Sterilization Requirements?
We ensure sterilization compatibility by design, validating materials and seals; we assess cleaning retries, and document cycle limits. We support clinical integration with validated interfaces, traceable QA, and clear guidance for hospital-grade sterilization requirements, procedures, and maintenance.
Can Ups-Level Surge Protection Be Integrated With Portable Power Units?
As in Odyssean returns, yes—ups level surge protection can be integrated with portable units. We, however, assess compatibility, wiring, and standards, focusing on portable integration while ensuring protection, reliability, and clear failure modes for reader guidance.
What Are the Data Logging Capabilities for Device Run-Time and Battery Health?
We provide data logging for device run-time and battery health. Our system records runtime events, charge/discharge cycles, voltage, and temperature, then analyzes trends to assess battery health and predict potential failures for proactive maintenance.
Do These Stations Meet NFPA 99 Critical-Care Electrical Safety Standards?
Yes, we meet NFPA 99 critical-care electrical safety standards, and we approach this with rigorous analysis. Portable standards and sterile integration are scrutinized, and we’ll document compliant paths, risks, and mitigations to assure reader confidence and safety.
How Quickly Can Portable Power Stations Be Replaced During Outages?
We can replace portable power stations within hours during outages. Our replacement timelines depend on availability and outage response planning, enabling rapid mobilization while maintaining critical care support. We’ll document steps, assign responsibilities, and monitor progress throughout replacement timelines.
Conclusion
We’ve seen how portable power stations can transform reliability across care settings, from monitoring to transport. By standardizing interfaces, prioritizing safety, and aligning with clinical workflows, we minimize downtime and maximize patient safety. The impact is immense—like a safety net for every shift. As we integrate these systems, we’ll tighten maintenance, optimize TCO, and assure real-time monitoring guides decisions. Together, we empower care with resilient power that never quits.

